-
INVICTA Group Services
chevron_left Backclose
INVICTA Group Services
- INVICTA Group
- INVICTA Clinics
- Medical Laboratories
- Fertility Bank
-
Anti-Aging Clinic
- R&D Centre
- Nami
Update date: 6 March 2026
Publish date: 9 June 2025
Read in: 8 min
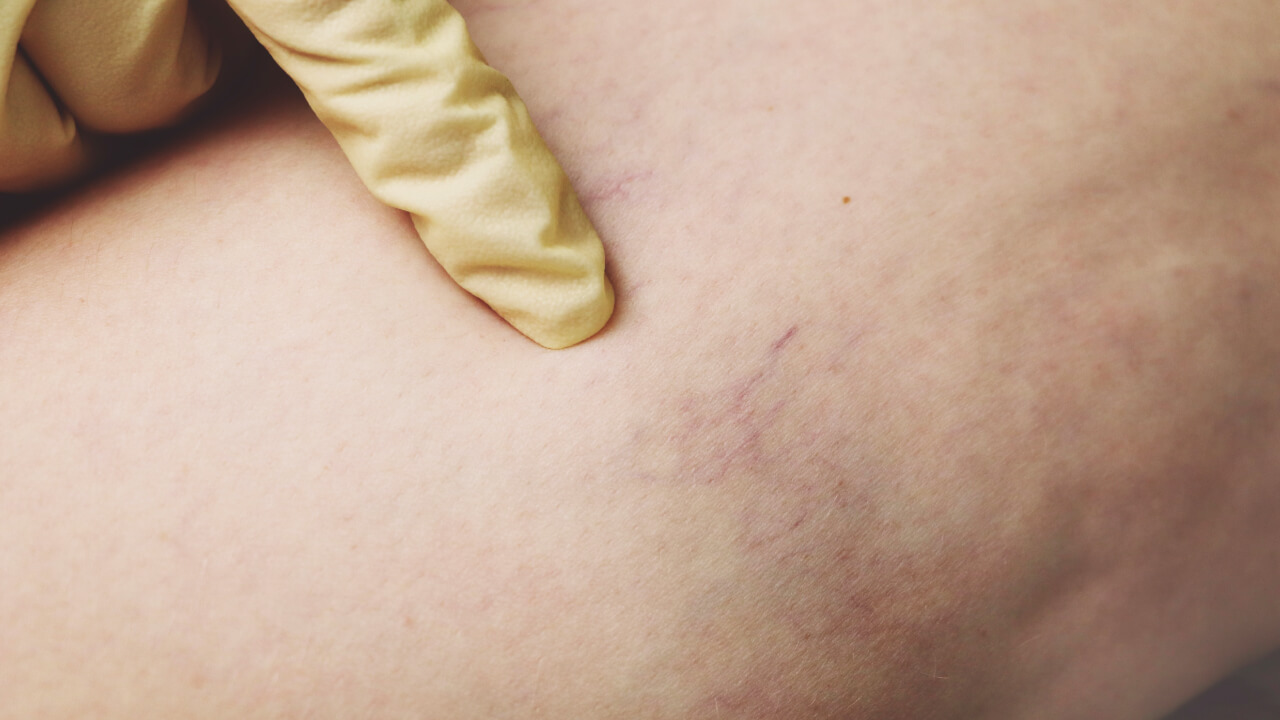
Broken capillaries can appear not only on the face but also on other parts of the body. This problem affects both women and men of all ages and is not merely an aesthetic concern. Why? Because broken capillaries on the legs may indicate venous insufficiency, while those on the face can be one of the first symptoms of rosacea or allergies. What causes broken capillaries and how can they be effectively treated?
Telangiectasias (commonly called spider veins) are web-like dilations of small blood vessels in the skin. Their diameter usually ranges from 0.1 to 0.4 mm, and they are located at a depth of approximately 0.4 mm.
In healthy individuals, blood vessels expand and contract depending on various conditions. If this mechanism is disrupted, weak and less elastic capillaries may rupture just beneath the epidermis, causing visible changes in the form of branching purple threads that create a characteristic network — hence the name “spider veins.” When present in large numbers, they may cause redness across a larger area of the skin.
This condition primarily affects women, regardless of age. This is related to estrogens (a group of female sex hormones), which relax the muscles of blood vessels, causing them to dilate. Broken capillaries are especially common in dry, thin, delicate skin with a pale tone and a pinkish tint — the so-called vascular skin.
These unaesthetic changes most often appear on the cheeks, nose, and décolleté. In these areas they usually take the form of red veins, while on the thighs and calves they tend to appear in a gray-blue color.
Common spider veins are divided into primary telangiectasias (associated with congenital diseases of the skin or internal organs) and secondary telangiectasias (related to external factors, systemic diseases, or skin conditions). They may appear anywhere on the body and at any age. Some people are particularly prone to developing them.
The main causes of broken capillaries include:
Genetic predisposition – if one of the parents struggles with this condition, there is a greater chance that the child may also develop it. In some individuals, capillaries run very close to the surface of the skin, which makes them more visible.
Lack of physical activity – both prolonged sitting and standing can put strain on the veins (especially in the legs). Therefore, telangiectasias (dilated capillaries) occur more often in people with sedentary jobs (e.g., office workers, drivers) or jobs that require standing (e.g., shop assistants).
Pregnancy – affects hormone levels, which increases the risk of spider veins. In addition, the amount of blood in the body increases during pregnancy, which can cause veins to enlarge. However, dilated blood vessels usually disappear on their own within about three months after childbirth.
Hormonal contraception – may be associated with various complications, including spider veins and varicose veins. Hormones contained in contraceptive pills can weaken the natural elasticity of venous walls.
External factors – extremely low or high temperatures, high humidity, strong wind, frequent use of tanning beds, and sun exposure increase the risk. Additional factors include chemicals, environmental pollution, and the use of topical steroids (especially on the face and décolleté).
Certain diseases – including diabetes, arterial hypertension, hormonal disorders, and rosacea. People with these conditions often experience spider veins.
Improper skin care – the use of unsuitable cosmetics containing strong fragrances or ethyl alcohol can promote the appearance of spider veins.
Certain dietary components – especially spicy foods and alcohol (alcohol consumption can lead to prolonged redness and rupture of blood vessels).
Age – although broken capillaries on the face or other areas may appear at any age, they most often occur before the age of 35 or after the age of 50.
Visible capillaries should never be ignored, as they may indicate serious changes in the venous system. Therefore, if we notice them on our skin, we should visit a doctor as soon as possible.
Treatment of broken capillaries mainly focuses on improving the appearance of the skin, and the choice of the appropriate therapy depends on the location and extent of the spider veins. Today, they are removed using modern treatments such as laser closure of broken capillaries. Under the influence of laser energy, small vascular lesions are sealed and become invisible. The condition of the skin after the procedure depends on the number and size of the spider veins and on how sensitive the patient’s skin is.
Sclerotherapy, on the other hand, is an effective method for treating varicose veins. During the procedure, a special substance is injected into the lumen of the blood vessel, causing its walls to close. The procedure produces visible results quickly and does not require hospitalization. However, during recovery it is recommended to wear compression tights or stockings.
Both laser capillary closure and sclerotherapy should be performed between autumn and spring. High temperatures are a contraindication for these procedures, mainly due to the need to wear compression dressings and, in the case of sclerotherapy, compression stockings, which may cause discomfort on hot days.
Cooler months are also the best time for laser therapy and sclerotherapy because patients must avoid sun exposure, saunas, and tanning beds for several weeks after both procedures.
People prone to broken capillaries on the face, legs, and other parts of the body should follow several recommendations that help prevent the appearance of unwanted spider veins. It is worth:
protecting the skin from UV radiation by using creams with UVA and UVB filters;
avoiding high-heeled shoes and shoes with narrow toes;
not overheating the skin (for example by taking very hot baths);
completely avoiding the sauna;
using rich protective creams during winter and rainy weather;
avoiding grainy scrubs and warming or drying face masks (the best choice is an enzyme peel designed for sensitive skin);
investing in high-quality cosmetics designed for vascular skin and using products that strengthen blood vessel walls;
supplementing vitamin C, which plays a role in collagen production in the body (collagen is responsible, among other things, for the elasticity and thickness of blood vessels);
avoiding alcohol, spicy foods, and quitting or significantly reducing smoking.
Read more